
For Megan Dursky, a registered nurse working in pediatrics in Cedar Rapids, Iowa, keeping perspective during COVID-19 has helped her perform to the best of her capabilities.
“When I do get scared – I think about how I would hope my child/nephew/niece would be taken care of when they are ill,” Dursky said. “What sort of treatment would I want for them? I then try to provide that for my patients.”

Megan and her husband, Trevor. Photo courtesy of Megan Dursky.
Dursky, whose husband Trevor serves in the Iowa National Guard, shares that when she first heard about the novel coronavirus, it seemed far away.
“Like many Americans, I did not think it would affect me personally, especially since I live in a rural area of the United States. I brushed it off for the most part and went about my normal routines of life. As I started to hear about how it was affecting Italy and began reading and seeing pictures of healthcare providers there — I started feeling uneasy — fearful of the unknown or what was to come.”
Almost immediately, Dursky began noticing changes in her day-to-day protocols at work.
“Things began to change in my workplace on a daily, and sometimes hourly, basis,” she shared. “Some of us wore paper masks while conducting patient care — others thought this was maybe a little over the top. We began to have daily, sometimes twice daily huddles to discuss new guidelines/procedures to implement. My work inbox began to fill with COVID-19 updates and our patients’ families began calling with questions regarding the outbreak. Things really sunk in when positive COVID-19 cases began to pop up locally in our communities and further PPE and protocols were put into place. By this point, our office was in the process of establishing a specialized clinic to receive patients with possible COVID-19 symptoms.”

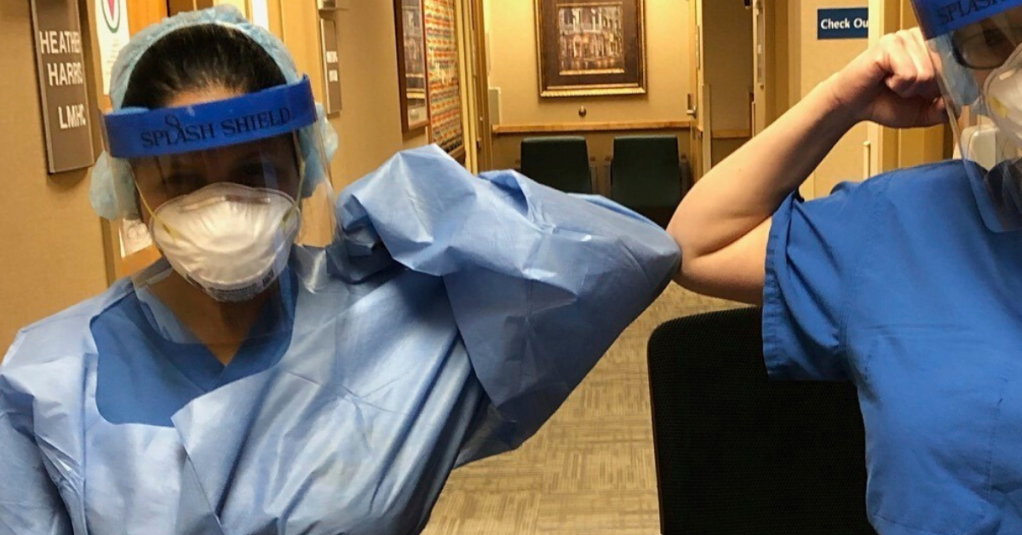
Dursky, left, in PPE. Photo courtesy of Megan Dursky.
While the threat of insufficient PPE looms and seeing stress on her co-worker’s faces happens more regularly, Dursky admits that working with families has sustained her in such an emotional and uncertain time.
“My favorite part of being a nurse is connecting with my patients and their families,” she said. “A high point for me is being able to educate them on ways to protect their families, keeping them as healthy as they can be during this difficult time. Providing reassurance that we will be available in the clinic to take their calls and questions; even as other services of the community are shutting down.”
While the nature of her job is to reassure the community, the thought of work coming home with her is never far from Dursky’s mind.

Megan and Trevor Dursky with their family. Photo courtesy of Megan Dursky.
“I’m fearful of contracting the virus myself and bringing it home to my family,” she shared. “Trying to serve patients while protecting those closest to me in my home. Every time you grab a door handle and then rub your forehead without thinking only moments later, have you just made a potentially life-changing mistake?”
Through it all, she says that nurses are truly there for patients.
“Without you — we would not be essential,” she said. “A smile from my patient can clear the day’s troubles from my mind and make everything we do worthwhile.”
We Are The Mighty will be featuring different heroes on the front lines of the battle with COVID-19. From health care workers to teachers, kind neighbors, grocery store employees and other mission essential personnel, if you know someone going above and beyond, please email us to feature them: tessa.robinson@wearethemighty.com.
