
It may come as a surprise to military personnel and civilians alike, but eye injuries are a serious problem in the U.S. military. Traumatic eye injury and other visual disorders from penetrating wounds rank fourth behind Traumatic Brain Injury (TBI), Post-Traumatic Stress Disorder (PTSD), and hearing loss as the most common injuries among service members in Operations Iraqi Freedom, Enduring Freedom and New Dawn.
On top of that, 75% of veterans who experience eye problems or traumatic brain injuries experience long-term visual dysfunctions, like light sensitivity and double vision. It’s an ongoing problem and will affect veterans for decades to come. There’s new work from the U.S. National Institutes of Health that could advance how we treat degenerative eye conditions in the United States.
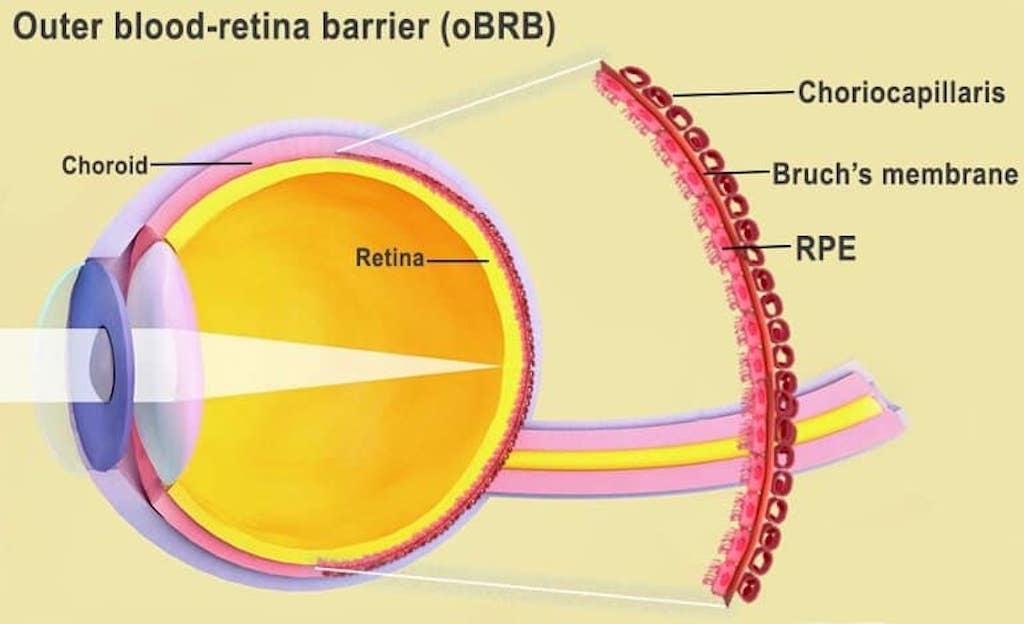
Scientists at the National Eye Institute (NEI) used patient stem cells and 3D bioprinting to create eye tissue that is advancing scientific understanding of just how these conditions continue to degenerate. Researchers printed a combination of cells that form the outer blood-retina barrier, an area of the eye that supports photoreceptors. This will allow future research to have an unending supply of tissue to study the effects of eye conditions and diseases.
A supply of tissue on which to experiment is critical to advancing medical research. In 1951, the study of cancer and potential treatments was stymied by the lack of sample cells from which to learn more about how cancer cells work and to test treatments. Cancer cell samples would die off quickly when taken to test laboratories. By happenstance, a woman named Henrietta Lacks walked into The Johns Hopkins Hospital one day.

Lacks complained of vaginal bleeding. Doctors found a malignant tumor in her cervix and took a sample of the cells for testing. Prominent cancer researcher Dr. George Gey’s tissue lab received the sample and made a miraculous discovery: Lacks’ cells didn’t die – they doubled every 24 hours. It created a nearly unending source of cell material from which to study the disease, its progression, and potential treatments.
Today, these cells (called HeLa cells) are still used to test the effect of everything from radiation and viruses to poison and vaccines, despite the fact that Henrietta Lacks died in October 1951. They were the first cells that could be shared and multiplied in a lab setting and have led to the eradication of Polio, the mapping of the Human Genome, and the HPV vaccine.
In creating the possibilities for 3D-printing of eye tissue in a laboratory setting, the NIH researchers have potentially uncovered an unending source of a kind of HeLa cell for eye tissue research. Their first tests using the tissue was studying the mechanics of age-related macular degeneration (AMD), where they were able to recreate the conditions that induced the causes of AMD.
Not only did this confirm theories surrounding the causes of AMD, it also showed that 3D-printed tissue works just like naturally-formed tissue. They are now experimenting with adding additional cell types to the printing process, such as immune cells.
The kind of foundational research conducted through this supply of eye tissue will allow further researchers to study the effects of other conditions, including many of which veterans suffer from as a result of their service. Just like the unforeseen advances made from Henrietta Lacks’ tissue research, the future possibilities of treating degenerative eye conditions is now wide open.
